We began our day in Chapel Hill with Dr. Robert Strauss, one of the high-risk obstetricians. Very comfortable, he explained the basics of the delivery procedure with heart condition babies. In our son's case, the delivery will be treated as normal until he's actually here...other than having ten doctors in the room when I actually deliver instead of the usual 2 or 3. We'll monitor his progress carefully over the remaining 7 weeks. Unless a delivery dilemma arises, there will be no need to induce or go to C-section due to our little boy's condition. As with most first time moms, I'll most likely go past my due date. If I've not begun labor within a week past March 1, they'll induce labor. Dr. Strauss is very committed to not acting preemptively so as to avoid unnecessary C-sections. I'll be having all remaining prenatal visits at UNC from here on out. Both Jordan & I were very comfortable w/Dr. Strauss. So our day started off very well.
Once we had finished w/Dr. Strauss, our care coordinator, Lisa Welborn, took us over to the Children's Hospital for our follow-up echocardiogram with Dr. John Cotton. Along the way, she familiarized us further on the hospital's layout as well as some possible financial programs to help with the cost of his surgeries. Lots of paperwork to go through. Lisa has arranged all our visits at UNC thus far & has been tremendously helpful. We were also updated of a follow-up sonogram for this Thursday at REX hospital. Since our son has a two-cord umbilical cord (normally, babies have a three-cord), doctors recommend a follow-up sonogram closer to delivery to measure the body, checking for any developmental hiccups or signs of problems. So we'll be seeing our boy again on Thursday! What a blessing to see him so often. This element has been one of the silver linings through this trying time as most mothers only have 1-2 sonograms their entire pregnancy. Thankfully, insurance has covered all 9 of ours!
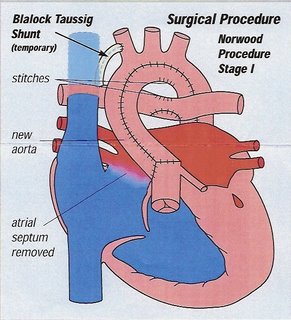
The fetal echocardiogram went very smoothly. The baby was positioned far more favorably this time, so Dr. Cotton was able to get a good view of his heart & how it has developed over the past 13 weeks. He confirmed the HLHS to still be there w/the atretic mitral valve & fibroelastosis of the left ventricle. However, no new complications have presented themselves either! So at this point, everything is on track for his first surgery during the week of his birth. The Norwood Procedure is the first of three open-heart reconstructive surgeries. In this procedure, the large main pulmonary artery & small aorta are fashioned together to make a new, larger aorta. There is a small tube (shunt) put in to connect the lung artery to the aorta. This shunt gives blood flow to the lungs. The wall that separates the top two heart chambers is then removed (atrial septectomy) to allow blood flow between the two atrium. The narrowing of the aorta is then opened & the connecting blood vessel removed. This procedure works to bypass the underdeveloped left ventricle & supply more adequate oxygenated blood to the body. Dr. Cotton reassured us again that though this procedure comes with the usual risks (70% success rate), he saw no indication from the echo that there is anything further going on that would jeopardize our boy's chances at this point.
Upon returning from a quick lunch on Franklin Street, Lisa took Jordan & me to tour the NICU. What a challenging place to be in. Most of the babies here are born prematurely & need constant high-risk care. Many of them were so small, even ranging to those born at 26 weeks! Lisa moved us through the hall fairly quickly so we would not have to dwell on all the tubes & machines connected to the tiny bodies that lay in the cribs. There is one attending physician for every 1-2 babies, keeping care constant & focused. Only 2 visitors are allowed in the room with the baby at a time due to space (as there are six infant stations to a pod), so it will be a juggling act for everyone to see our boy once he's here. The same visiting limit is true for the PICU as well. The babies receive 24-hour care here. Our son will go from the delivery room to the NICU for the days up until his first surgery. Following his surgery, he'll receive care in the PICU (more to come on that later).
After our tour of the NICU, we met with neo-natalogist, Dr. Marty McCaffery. What a delightful man. He talked us through the days between our baby's birth & going into surgery. He'll be one of the four neo-natal physicians in the delivery room with us when our boy arrives on the scene. Our time with Dr. McCaffery was very helpful as he gave us more insight on what our boy's time in the NICU may look life. Babies with HLHS are put on the medication prostaglandin to keep the ductus arteriosis open, thus allowing oxygenated blood to get to the body. There is often a balancing act involved with babies on prostaglandin as they need to get adequate oxygen (often through ventilator) though not so much as to overwhelm the lungs. Sometimes, the neo-natalogists will need to give these babies nitrogen to keep oxygen levels in the lungs around 70-80% SAT. Once the baby has successful transitioned over from newborn circulation, he'll undergo the first open-heart surgery. These babies also receive IVs through their umbilical cord to ensure adequate nutrition & medication as needed. Every baby is different, so the staff of the NICU provides 24 hour care for tailored care to each infant. We were so pleased w/Dr. McCaffery. He spoke directly with us about what care may be necessary during our boy's stay in the NICU while educating us along the way. He was also quite compassionate & by the end of the meeting, we not only had another doctor on our side, but a friend.
Our day came to a close with tours of both the Labor & Delivery floor and the PICU. Lisa was very helpful in getting us acquainted with the Labor & Delivery floor, showing us delivery, triage, & waiting rooms. This wing is just down the hall from the NICU, making our boy's trip from one place to the next quick & efficient. Being a high-risk patient, I'll be strapped up to multiple monitors & equipment during my time at L&D. The room will be quite crowded by the time of delivery, with up to ten different doctors & attendees in the room. This is to ensure the quickest response for our boy should he come out in a traumatized state. However, if he comes out pink & doing well, we'll be able to hold him for a few minutes before they take him to the NICU.
Finally, we toured the PICU. This proved to be the most difficult portion of our day. Every child in PICU has their own room, in part because of the size of all equipment needed. About 30-40% of the children in the PICU at any given time are surgery patients from Dr. Mills, so they are well acquainted with open heart & transplant patients. While the patients here were not nearly as small as those in the NICU, it was more difficult to take as you could see them more clearly in their rooms (the NICU babies could barely be seen over the cribs & equipment). So many of the children were either sleeping or looked worn out, plugged in to several monitors & tubes. A grandmother was rocking a little baby in one room...he looked so small & tired. It is amazing how much some of these children go through so early on in life. Lisa moved us through this portion of the day fairly quickly so as not to dwell too long on the condition of these children. What a blessing to have facilities like this for children who need such delicate & attentive care! Our boy will stay in the PICU when recovering from surgery & then will be moved to the CICU (Cardiac Intensive Care Unit), where everyone is fully acquainted with heart patients & surgeries.
So our day at UNC was a success. Jordan & I are now more acquainted with the specifics of our boy's care once he's here, as well as how to get to everything in the hospital. He was definitely my strength during the difficult moments of the day, taking my hand & giving reassuring hugs & kisses just when I needed them most. He has been absolutely amazing through this whole journey, constantly reminding me in my weak moments that our great God is in control & that everything will be fine, no matter what that means. Some days, he'll just hold me close & whisper, "I'm here. We're going to get through this together. God is in control." What an amazing man!
Thank you all again for your many prayers on our behalf. Its shocking to realize that March 1st is just 6.5 weeks away! Keep checking back as updates will be coming more quickly now. This sweet boy of ours is growing big & strong...some days, I wonder how I'll be able to keep up as it seems I'm stretched to the limit already. Pregnancy certainly is a fascinating experience. Here's wishing you all a delightful day! And again, many thanks!
9 comments:
Pastor Gary gave a sermon on Abraham last Sunday. How his belief was counted to him as righteousness by God. May you be as blessed as Abraham.
Much love - Miss Kateri
I'm learning so much from your blog! Your mind must be swimming with facts and knowledge about every aspect of this pregnancy. Praise the Lord for your strength through all of this. I will be praying for a pink little baby so you can hold him before the surgery.
You guys are an awesome example to us all of Jesus' love and faithfulness. We are praying for the 3 of you.
Hey, Jordan and Patience. This is Danielle Renstrom (Adam and Nat's sister-in-law). Thanks for keeping your blog up-dated on baby Leino. Glad to hear Friday went well. I sure will be praying for a safe, healthy delivery for your little boy, and that the Lord will give you joy and peace each step of the way.
Hey patience and Jordan,
Your in prayers! I'm blubbering over here from reading your blog. Maybe it's the 48 hour thing at church thats so graciously running over it's preplanned hours lol, but to think that God is sitting there right now, smiling upon baby J. He already knows his name, he already knows his plan in life. And if he is anything like his parents, that is going to be one phenomenal kid! We dont know what God has planned but we know He said, His plans for us are good and true.
I love you guys, thank-you for being an inspiration, you truly lead by example.
Love- Christal
Patience,Jordan,and baby Leino,
What an amazing journey of faith and love. Jordan thank you for being the kind of man of faith and husband of quiet strength for our precious Patience.
Wonderful daughter, know that all around the world people are thanking God for your witness and your willingness to allow us all to share in both the wonder and the worry so normal as you sit in God's waiting room.
Be encouraged also that your blog that is being resent all over the world is producing healing miracles of the heart as people are being broken free of the scar tissue of hurt and pain that can hinder all of us from the joy and blessing God has waiting for us all as His children.
At church Sunday I sat near a family of 5 kids. The little 3 year old boy had the same condition at birth and he had the same proceedures done and he was doing great...climbing all over everything with a huge smile on his face...I smiled right back at him and with a tear said a quiet prayer of thanksgiving that Jesus your ways may be a mystery...but you are good and your journey Patience and Jordan and your little boy will bear witness to His Glory.
Lots of love,
Dad (Roddy)
Patience and Jordan,
I just wanted to wish you all the best and let you know you are in our prayers. I did have a little bit of information that might be helpful, don't really know how much but I have a close relative who works at UNC's children's hospital on the medical/surgical floor. If you would like to get in touch and see if there is any additional info or questions. Just let me know what I can do.
We will be praying.
Patience and Jordan,
What a fasinating journey you are on! Only the Lord knows what lies ahead but we do have assurance He will not give you more than you can endure. Your prescious son has been safe within you thus far and when the time comes to turn him over to the excellent staff you have informed us of, we know the Lord will accompany him on. You are a special threesome and are loved. Gods' blesssings. Love, Naomi
Patience and Jordan,
My family is praying for yours and a successful surgery today. Your resilience is truly amazing - let's see some miracles today and in the future!
Post a Comment